Seasonal Allergies: Naturopathic Management
The warm weather does not only signal that summer is on its way, but that the pollen is out! Allergy sufferers worldwide understand this love-hate relationship with spring and summer. My personal experience with allergies as an adolescent drew me to naturopathic medicine. Through nutrition, supplements, herbal medicine, and other lifestyle strategies, I no longer rely on antihistamines like I once did. Allergic rhinitis lends itself well to the incorporation of both holistic and mainstream approaches, as many naturopathic treatments will not interact negatively with pharmaceutical treatments if needed, especially acupuncture and dietary recommendations.
Allergic Responses
Pollen is recognized by the body of allergic individuals as a foreign antigen (invader), causing the immune system to start an inflammatory cycle. This involves the immune system to recruit mast cells (defenders) in response to the antigen. Mast cells release histamine which leads to more blood flow directed to the area where the pollen is (e.g., nose, eyes, throat), causing ongoing allergy symptoms such as:[1]
- Sneezing, congestion
- Itching: nose, eyes, ears, palate
- Bronchial irritation
- Postnasal drip
- Fatigue, drowsiness, malaise
- Dark under-eye circles
If left unmanaged, allergic rhinitis can lead to sinusitis, otitis media, sleep apnea, and eustachian-tube dysfunction.
Conventional Treatments [1]
Conventional treatments involve controlling environmental exposure to known allergens (e.g., pollen, dust mites, mold), and use of medications such as pharmaceuticals and immunotherapy. Pharmaceutical antihistamines aim to prevent the immune response from getting out of control, by targeting the molecule histamine. Over the counter antihistamines, decongestants, and nasal sprays (steroids) are most commonly used. Medication side effects include dry mouth, headache, drowsiness, and rebound congestion (this may occur with over-usage and long-term dependence on antihistamines).
 Lifestyle Strategies
Lifestyle Strategies
Both medical doctors and naturopathic doctors choose first to do no harm. This means starting with the basics such as closing windows to avoid pollen buildup, dusting, using HEPA/air purifier filters, washing of linens containing allergens, and frequent washing of bedding, just to name a few.[1]
Other basic “antiallergy strategies” start with a healthy diet rich in antioxidant and anti-inflammatory foods. This change is not elaborate but supports eating large servings of fruits and vegetables, choosing more lean proteins/fish over processed meats, healthy fats (e.g., avocado, coconut oil, olive oil), and spices like turmeric and ginger that target inflammation. Packaged foods with high fat and sugar promote congestion and inflammation, leading to more allergy symptoms. So, try reducing processed foods and sugars when possible. Milk and dairy consumption may also worsen mucous formation, therefore worsening nasal congestion.
Stress reduction helps the body better tolerate excess antigens (the pollen “invaders”), allowing your body to have less of an immune response. Try some yoga, meditation, or go for a walk to help promote healthy breathing and aid in relaxation.
Naturopathic Supplements and Herbs
Research shows that some naturally occurring plant compounds have antihistamine effects. Naturopathic supplements including probiotics, vitamin C, quercetin, and nettle work to reduce inflammatory pathways related to allergies.
Quercetin
This compound is a flavonoid (plant antioxidant) that has been shown to have both antiallergy and anti-inflammatory effects in animal and human research models.[2] Foods that are high in quercetin are capers, onions, apples, and dark red or blue berries.
Vitamin C
Ascorbic acid, the active constituent in vitamin C, has been found to lower histamine concentrations in the blood of patients with allergic diseases.[3] From this, we can gather that vitamin C possesses antihistamine activities, similar to a pharmaceutical version. Vitamin C is found in a plethora of foods like bell peppers, dark leafy greens, broccoli, and citrus fruits.
 Nettle (Urtica dioica)
Nettle (Urtica dioica)
This plant, also known as “stinging nettle” due to its small spikes, has many uses and has shown promise in allergy reduction. A cell study found that nettle was an antagonist of histamine receptors (basically inhibiting the receptor stimulation) and inhibited inflammation.[4] Nettle can be found in the form of tea leaves or an herbal tincture. You can forage nettle outdoors, but you should know how to properly handle the stinging leaves.
Probiotics
Probiotics used early in life may work preventatively to reduce allergy incidence in adolescence and onwards. Evidence shows that the gut controls various immune-system functions, so using probiotics can help reduce the body’s allergic response. Early childhood uses of probiotic strain Lactobacillus rhamnosus (daily by mother from 35 weeks gestations to 6 months postpartum while breast-feeding, and then from birth to 2 years of age) prevented atopic sensitization (allergies, eczema) and hay fever prevalence later in life.[5]
Other mentionable supplements used in naturopathic medicine for control of allergy symptoms are bromelain; omega-3 fatty acids; and other herbs such as astragalus, reishi, and eyebright.
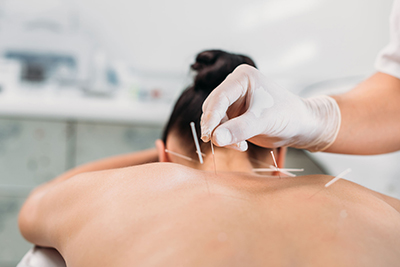 Acupuncture
Acupuncture
It is thought that acupuncture may positively benefit the immune system, therefore may have a positive impact on allergic rhinitis (allergies). A meta-analysis found that compared to the control group (no acupuncture), the acupuncture treatment group showed a significant reduction in the following:[6]
- Nasal symptoms
- Use of medication
- Quality-of-life scores
- IgE levels in the bloodstream, which is a measure of allergic responses in the body
There is an abundance of literature regarding the specific acupuncture points that have been shown to benefit allergic rhinitis. A randomized controlled trial found that several acupuncture sessions involving a series of specific acupuncture points reduced the number of days that an antihistamine was required.[7] In this study, acupuncture points such as L14, LI11, Yintang, Bitong, LU7, SP6, and ST36, among others, were used for allergy control.[7] Acupuncture protocols involving points over top of the sinus area (Yintang, Bitong), and on other parts of the body, may also reduce antihistamine dependence and allergic symptoms. Both LI4 and LU7 are important points, controlling aspects of the face and lung/respiratory system. Acupuncture has shown the potential ability to limit reliance on antihistamines for allergic rhinitis management, and to reduce antihistamine and other drug-induced side effects that can also affect quality of life.
Conclusion
Including both naturopathic and lifestyle techniques in your seasonal allergy regiment can be helpful in reducing reliance on antihistamines and nasal decongestants and provide more long-term relief.
 Kaitlyn Zorn, HBSc, ND
Kaitlyn Zorn, HBSc, ND
A Guelph naturopathic doctor who uses a blend of modern science and traditional healing therapies to treat the whole person. Her journey has helped her develop an interest in brain health, pain management, and critical illness relief.
drkaitlynzornnd.com
References
- Medscape. Allergic rhinitis. https://emedicine.medscape.com/article/134825-overview · Updated 2018-01-26.
- Chirumbolo, S. “The role of quercetin, flavonols and flavones in modulating inflammatory cell function.” Inflammation & Allergy Drug Targets, Vol. 9, No. 4 (2010): 263–285.
- Hagel, A.F., C.M. Layritz, W.H. Hagel, H.-J. Hagel, E. Hagel, W. Dauth, J. Kressel, et al. “Intravenous infusion of ascorbic acid decreases serum histamine concentrations in patients with allergic and non-allergic diseases.” Naunyn- Schmeideberg’s Archives of Pharmacology, Vol. 386, No. 9 (2013): 789–793.
- Roschek, B. Jr, R.C. Fink, M. McMichael, and R.S. Alberte. “Nettle extract (Urtica dioica) affects key receptors and enzymes associated with allergic rhinitis.” Phytotherapy Research, Vol. 23, No. 7 (2009): 920–926.
- Wickens, K., C. Barlow, E.A. Mitchell, J. Kang, N. van Zyl, G. Purdie, T. Stanley, et al. “Effects of Lactobacillus rhamnosus HN001 in early life on cumulative prevalence of allergic disease to 11 years.” Pediatric Allergy and Immunology, Vol. 29, No. 8 (2018): 808–814.
- Feng, S., M. Han, Y. Fan, G. Yang, Z. Liao, W. Liao, and H. Li. “Acupuncture for the treatment of allergic rhinitis: A systematic review and meta-analysis.” American Journal of Rhinology & Allergy, Vol. 29, No. 1 (2015): 57–62.
- Adam, D., L. Grabenhenrich, M. Ortiz, S. Binting, T. Reinhold, and B. Brinkhaus. “Impact of acupuncture on antihistamine use in patients suffering seasonal allergic rhinitis: Secondary analysis of results from a randomised controlled trial.” Acupuncture in Medicine, Vol. 36, No. 3 (2018): 139–145.

 Stores
Stores