What Does It Mean to Be Adrenal-Fatigued? Naturopathic Assessments and Supports
These days, it is quite rare to meet someone who does not identify with fatigue or stress on some level. Adrenal insufficiency is a common diagnosis amongst naturopathic doctors and alternative practitioners, but few will fully investigate the extent of the insufficiency and determine the right herb for the right person.
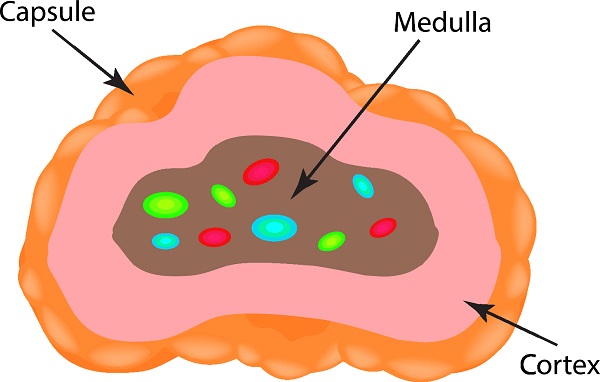
If we take a deeper look at the adrenal anatomy, we know there is a cortex and medulla which are each responsible for producing a certain set of hormones. The cortex, or outer layer of the adrenal gland, releases aldosterone (important for regulating salt balance), cortisol (our main stress hormone), and a certain amount of androgenic hormones DHEA and testosterone. The inner medulla is responsible for releasing our catecholamines, or “fight-or-flight” hormones, such as adrenaline and noradrenaline.[1]
So, what does it mean to be adrenal-fatigued? According to endocrinologists, there are four stages of adrenal fatigue, and each is characterized by a hormone profile measured through the blood.
 The first stage is the “Initial Alarm Phase,” in which the body is faced with a short-term immediate stressor, such as a job interview or high-pressured exam. At this point, the body is fully capable of creating the necessary hormones in adequate amounts to meet the demands. All you may notice is an increased alertness, perhaps a slightly increased heart rate. If your hormones levels were to be measured in your blood, your adrenaline, noradrenaline, cortisol, and insulin levels may be slightly elevated. This stage appears fairly benign, and is one we often move in and out of during a regular day living and working in North America.[2]
The first stage is the “Initial Alarm Phase,” in which the body is faced with a short-term immediate stressor, such as a job interview or high-pressured exam. At this point, the body is fully capable of creating the necessary hormones in adequate amounts to meet the demands. All you may notice is an increased alertness, perhaps a slightly increased heart rate. If your hormones levels were to be measured in your blood, your adrenaline, noradrenaline, cortisol, and insulin levels may be slightly elevated. This stage appears fairly benign, and is one we often move in and out of during a regular day living and working in North America.[2]
 The second stage is known as the “Continual Alarm Phase,” in which the stressor is around for a longer period and the demand for stress hormone is sustained. At this time, bloodwork would likely show a higher level of cortisol, but a declining level of DHEA and testosterone. All resources are shifted towards making cortisol, which means the production of sex hormones become less of a priority. Someone in this stage of adrenal health may notice they are very focused and alert during the day, but as soon as they are finished work or a difficult task, they crash and can barely function the rest of the day. These people are often “tired but wired” and struggle through the rest of the day, or turn to energy drinks for support.
The second stage is known as the “Continual Alarm Phase,” in which the stressor is around for a longer period and the demand for stress hormone is sustained. At this time, bloodwork would likely show a higher level of cortisol, but a declining level of DHEA and testosterone. All resources are shifted towards making cortisol, which means the production of sex hormones become less of a priority. Someone in this stage of adrenal health may notice they are very focused and alert during the day, but as soon as they are finished work or a difficult task, they crash and can barely function the rest of the day. These people are often “tired but wired” and struggle through the rest of the day, or turn to energy drinks for support.
 The third, “Resistance,” phase of adrenal fatigue can last many months or even years. In this phase, the demand for stress hormone is even greater and prolonged. The body is putting all its effort into shunting resources from areas of lesser significance to make more cortisol. The most noticeable change on bloodwork will be lower levels of DHEA, testosterone, and even progesterone, resulting in changes in menstrual cycle and lowered sex drive. The fatigue will weigh in no matter what time of day, and new symptoms may include a decrease in enthusiasm, motivation, and mood. A common finding for practitioners is the constant feeling of a low-grade cold/flu, possibly even coupled with swollen lymph nodes around the neck and a decreased body temperature.
The third, “Resistance,” phase of adrenal fatigue can last many months or even years. In this phase, the demand for stress hormone is even greater and prolonged. The body is putting all its effort into shunting resources from areas of lesser significance to make more cortisol. The most noticeable change on bloodwork will be lower levels of DHEA, testosterone, and even progesterone, resulting in changes in menstrual cycle and lowered sex drive. The fatigue will weigh in no matter what time of day, and new symptoms may include a decrease in enthusiasm, motivation, and mood. A common finding for practitioners is the constant feeling of a low-grade cold/flu, possibly even coupled with swollen lymph nodes around the neck and a decreased body temperature.
The fourth and final stage of fatigue is known as the “Burnout” phase. We often throw this word around when discussing students writing exams, individuals going through divorce, or parents with young children. However, bloodwork at this time will show a whole different level of burnout, which includes very low levels of all hormones produced by the adrenal glands. This includes cortisol levels, adrenaline, testosterone, DHEA, and aldosterone. At this point, the body has run out of resources, can no longer meet the demands placed on it, and has begun to crash. Depression, anxiety, irritability, weight loss, apathy, absent sex drive, poor sleep, and frequent infections plague a burned-out individual in ways so severe that they are nearly nonfunctional. Needless to say, this stage should be fairly obvious to the individual, but even then, people ignore it, struggle to step back from their day-to-day lives and recover or are just unaware of the gravity of their situation. As with all chronic conditions, the burnout phase is not cured overnight, and can take months of dedicated treatment, paired with permanent lifestyle changes to see a full recovery.
So, What Is the Best Way to Manage Someone With Adrenal Fatigue or Insufficiency?
An adrenal treatment plan will vary depending on many factors, including the phase of fatigue, the individual’s diet, exercise, sleep, and intensity of stressors. Ideally, each assessment begins with a detailed intake of these things as well as a workup of the most common early-screening blood tests. Each individual should have a fairly recent screen for a full thyroid panel, inflammatory factors (ESR, CRP), iron, HbA1C, fasting insulin, and tests for liver and kidney function. Salivary cortisol should be considered whether as a one-point or four-point cortisol test, in order to monitor how cortisol fluctuates over the day and if it is consistent with energy levels.[3]
Physical exams for adrenals are never fully objective, but assessments of pupillary reaction, conjunctiva, thyroid, hair, skin, and nails should be considered. Because cortisol plays an important role in weight management, blood-sugar control and cravings, waist-to-hip ratio, body composition analysis, and overall weight can be an integral part of measuring progress.
Once a diagnosis of adrenal insufficiency can be confirmed, there are a number of treatments to implement before any supplementation can be considered. Beginning with diet, all meals should be whole-food–based and strictly avoid refined sugars, energy drinks, and caffeine—all of which will stress the immune system more and place an increased burden on the adrenal glands. Alcohol as a depressant will not do much for energy, and will instead contribute to nutrient depletion and gastrointestinal inflammation. If the patient has known food sensitivities, it is wise to avoid these foods and simplify the diet as much as possible.
 Many patients will not have the energy to continue an exercise plan, but it is an important part of creating routine for the body and ensuring balance if done in the right way. Exercise should be less than 45 minutes in length and include low-intensity cardiovascular activity such as a treadmill or elliptical. Resistance training can be included at lower weights and with higher repetitions. In addition to these lifestyle recommendations, patients should consider a sleep log or a tracking device such as a FitBit or smartphone app to monitor restlessness during the night. For stressors that are difficult to avoid, a counsellor should always be considered as part of the stress-management plan.
Many patients will not have the energy to continue an exercise plan, but it is an important part of creating routine for the body and ensuring balance if done in the right way. Exercise should be less than 45 minutes in length and include low-intensity cardiovascular activity such as a treadmill or elliptical. Resistance training can be included at lower weights and with higher repetitions. In addition to these lifestyle recommendations, patients should consider a sleep log or a tracking device such as a FitBit or smartphone app to monitor restlessness during the night. For stressors that are difficult to avoid, a counsellor should always be considered as part of the stress-management plan.
Supplements to Consider
Digestive health should be considered in the first-line treatment of any health concern, especially adrenal fatigue. Monitoring regularity of bowel movements and all signs of indigestion ensures that nutrients are being digested and absorbed properly, increasing the patient’s potential to see noticeable changes in energy as soon as possible. This treatment can include digestive enzymes, probiotics, magnesium, or other gastrointestinal supports as seen fit by the practitioner.
 Adaptogenic herbs are plants with the potential to lower cortisol levels and support the body in its adaptation to stress. They are exceptionally effective at promoting energy levels, encouraging sleep, lifting mood, and preventing illness if the right herb is chosen for the right person. There are a number of combination adrenal supports, but they do not work for everyone and can often leave some depleted individuals feeling anxious and jittery. A few of the most common adrenal supports include:
Adaptogenic herbs are plants with the potential to lower cortisol levels and support the body in its adaptation to stress. They are exceptionally effective at promoting energy levels, encouraging sleep, lifting mood, and preventing illness if the right herb is chosen for the right person. There are a number of combination adrenal supports, but they do not work for everyone and can often leave some depleted individuals feeling anxious and jittery. A few of the most common adrenal supports include:
- Withania: It is also known as ashwagandha and is an Indian herb with implications in thyroid health and adrenal support. Withania works for every stage of adrenal fatigue, but has best effects on the second and third phase, increasing focus, calming the mind, and supporting the immune system in just a matter of days.[4]
- Rhodiola: This herb has a great benefit in the third and fourth phases of adrenal fatigue because of its uplifting effects on mood, enthusiasm, and motivation. This herb is best taken in the early parts of the day and is most effective in combination with St. John’s wort and Panax ginseng.
- Eleutherococcus: It is also known as Siberian ginseng and is a common part of many combination adrenal formulas. It is helpful in the third and fourth phases of fatigue because it supports the immune system and reduces the frequency of infections. With less of an impact on the mental-emotional side of things, Eleutherococcus can be used with other medications and can also be consumed in tea form.
- Glycyrrhiza: We know this one commonly as licorice and often add it to liquid herbal formulas to improve taste. Glycyrrhiza has a tremendous impact on adrenal health, but often gets a bad wrap because it can increase blood pressure and can be overstimulating for the later stages of adrenal fatigue. To increase its effectiveness, use in combination with other herbs and monitor blood pressure and cortisol levels.
Other than these specific adrenal herbs, supplements for general health and energy should be fortified in the short term. These include all B vitamins, vitamin D, zinc, magnesium, iron, and vitamin C. For the best combination of herbs and vitamins for your specific adrenal picture, please consult with your naturopathic doctor and get on your road to recovery!
References
- Society for Endocrinology. “Adrenal glands.” You and your hormones · http://www.yourhormones.info/glands/adrenal-glands/ · Updated 2018-01.
- Hansen, F. “The four stages of adrenal fatigue.” The Adrenal Fatigue Solution · https://adrenalfatiguesolution.com/stages-of-adrenal-fatigue/ · Updated 2018.
- Prousky, J. “Adrenal fatigue.” In Textbook of integrative clinical nutrition, 88–90. Toronto: CCNM Press, 2012.
- Chandrasekhar, K., et al. “A prospective, randomized double-blind, placebo-controlled study of safety and efficacy of a high-concentration full-spectrum extract of ashwagandha root in reducing stress and anxiety in adults.” Indian Journal of Psychological Medicine, Vol. 34, No. 3 (2012): 255–262.

 Stores
Stores
 Dr. Krysten DeSouza, ND
Dr. Krysten DeSouza, ND